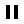Anterior Hip Replacement
Direct anterior total hip arthroplasty or replacement is a minimally invasive hip surgery performed to replace the total hip joint without cutting through any major muscles. It is also referred to as muscle sparing surgery because no major muscles are cut enabling a quicker return to normal activity.
Traditionally with total hip replacement, the surgeon makes the hip incision laterally, on the side of the hip, or posteriorly, at the back of the hip. Both approaches involve cutting major muscles to access the hip joint. With the direct anterior approach, the incision is made in front of the hip enabling the surgeon to access the joint without cutting though any major muscles.
Indications
Hip replacement is indicated in patients with arthritis of the hip joint.
Arthritis is a condition in which the articular cartilage that covers the joint surface is damaged or worn out causing pain and inflammation. Some of the causes of arthritis include:
• Advancing age
• Congenital or developmental hip diseases
• Obesity
• Previous history of hip injury or fracture
• Increased stress on hip because of overuse
Symptoms
Patients with arthritis may have a thinner articular cartilage lining, a narrowed joint space, presence of bone spurs or excessive bone growth around the edges of the hip joint. Because of all these factors arthritis patients can experience pain, stiffness, and restricted movements.
Diagnosis
Your doctor will evaluate arthritis based on the characteristic symptoms and diagnostic tests. Your orthopedic surgeon will perform a physical examination, order X-rays and other scans, and also some blood tests to rule out any other conditions that may cause similar symptoms.
Procedure
Direct anterior total hip replacement surgery involves the following steps:
• The procedure is performed under general anesthesia or regional anesthesia.
• You will lie down on your back, on a special operating table that enables the surgeon to perform the surgery from the front of the hip. Your surgeon may use fluoroscopic imaging during the surgery to ensure accuracy of component positioning and to minimize leg length inequality.
• Your surgeon will make an incision, about 4 inches long on the front of the hip. The major muscles are pushed aside to gain access to the joint and perform the replacement.
• Next, the femur bone is separated from the acetabular socket.
• The acetabular surface is prepared using a special instrument called a reamer.
• The acetabular component is cemented or fixed with screws into the socket.
• Then a liner made up of plastic, metal, or ceramic is placed inside the acetabular component.
• The femoral head that is worn out is cut off and the femur bone is prepared using special instruments so that the new metal component fits the bone properly.
• Then the new femoral component is inserted into the femur bone either by press fit or by using special bone cement.
• The femoral head component made of ceramic or metal is then placed on the femoral stem.
Post-operative care
After traditional hip replacement surgery, you would be instructed to follow hip precautions to prevent your new hip from dislocating. These guidelines are very restrictive and include no bending or flexing the hip past 90 degrees, no crossing of legs, use a pillow between the legs when sleeping, and use an elevated toilet seat.
With the anterior approach you will not have to follow standard hip precautions.
Your doctor will however give you instructions to be followed at home for a faster recovery. These include:
• Take medications as prescribed to relieve pain and prevent infection
• Participate in physical therapy to restore hip function and strength
• Eat a healthy diet and do not smoke to facilitate healing and promote a faster recovery.
Contact your doctor if you observe increasing swelling or redness in the operated area.
Risks and complications
All surgeries carry an element of risk whether it is related to the anesthesia or the procedure itself. Risks and complications are rare but can occur. Below is a list of complications that can occur following any hip replacement procedure:
• Infection at the incision site or in the joint space
• Fracture
• Nerve damage
• Hemarthrosis-excess bleeding into the joint after the surgery
• Deep vein thrombosis (blood clot)
• Leg length inequality